In this month’s alert
Humanising Healthcare’s Conversation Café: transforming medical education – podcast feature
Scotland faces the highest drug-related death rate in Europe, and one of the highest alcohol death rates, yet its recovery communities are thriving. Humanising Healthcare’s Conversation Café bridges these worlds, bringing medical students together with people with lived experience of addiction for two-hour, round-table discussions. Speaking on IAS’s podcast, Dr Hugo Jobst said:
Historically in medical education the roots of addiction have not really been discussed in any meaningful or effective way. You know they’ll say, ‘adverse childhood experiences increase your risk of addiction’, but you haven’t actually heard from anyone who’s actually had those adverse childhood experiences. So with this, students get a true experience by hearing a story and being able to connect with someone who has gone through that.
The Cafés start with a short personal story from someone in recovery, then students rotate through small-group discussions guided by questions such as “What are the roots and origins of addiction?” and “How can healthcare professionals support harm reduction?” The sessions encourage empathy, challenge stigma, and give students insights rarely taught in traditional medical curricula.
Since its launch, over 300 students across four Scottish medical schools have participated. Endorsed by the Scottish Government, the project is now part of Dundee and Glasgow’s curricula. By connecting future doctors with recovery communities, Conversation Cafés are shaping a more compassionate, human-centred approach to addiction medicine.
If you’re interested in setting up a Conversation Café at your institution, contact: humanisinghealthcare@gmail.com
You can see how the Cafés run in the following short film:
Alcohol deaths in Northern Ireland highest in the UK, prompting calls for MUP
There were 397 alcohol-specific deaths in Northern Ireland in 2024 – a record high, up from 341 in 2023, and a rise of 81% since 2014.
This means Northern Ireland has the highest alcohol death rate (21.4 per 100,000) across the whole of the UK, despite having less than half of Scotland’s rate a decade ago.
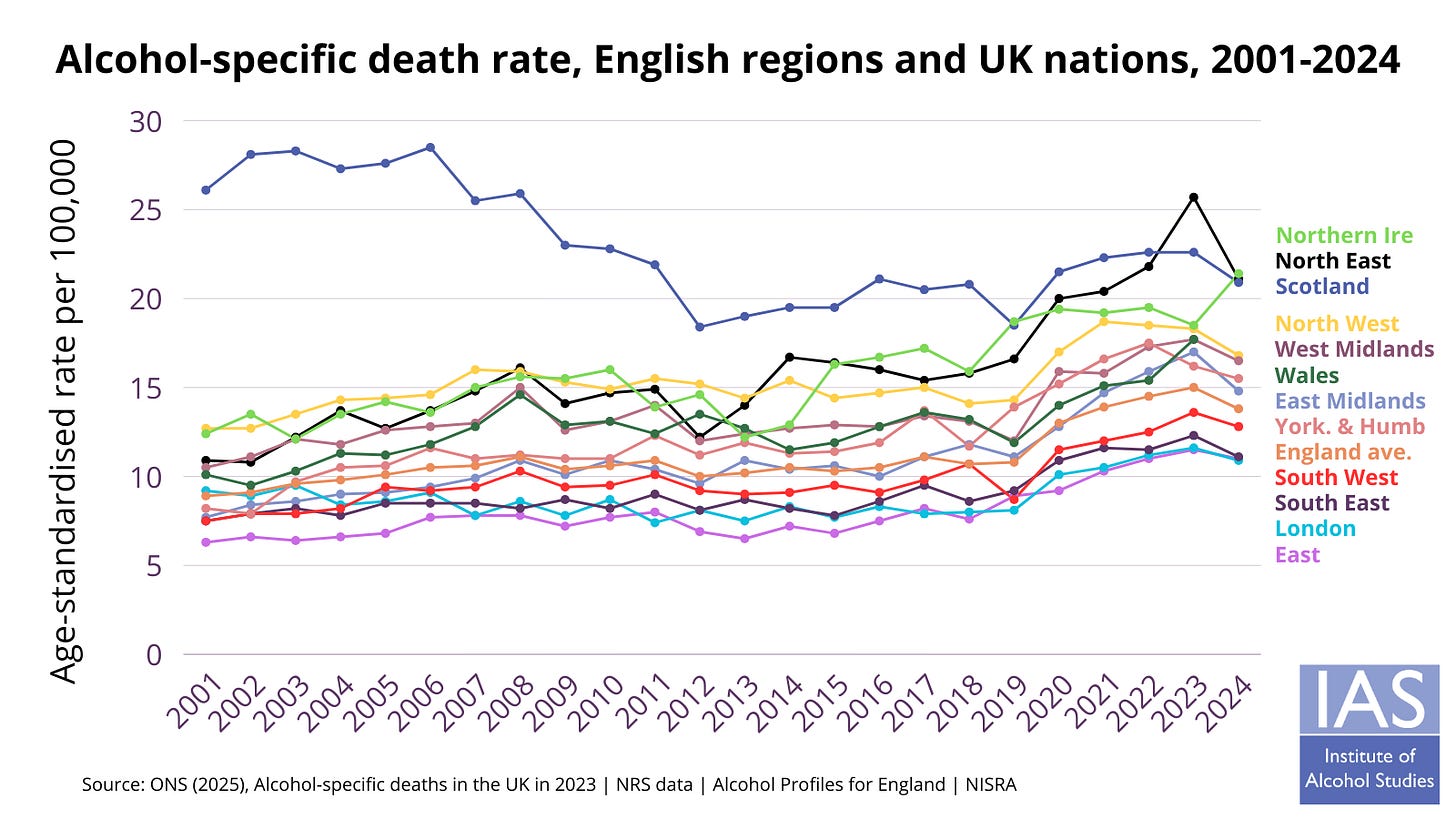
The death rate was almost double for men, at 28.1 compared to 14.9 for women, and deaths were highest among people aged 45-54 and 55-64.
Between 2020 and 2024, the percentage of alcohol-specific deaths in Northern Ireland’s most deprived areas (36.7%) was almost four times that of the least deprived areas (9.9%).
Dr Clodagh Corrigan of the British Medical Association’s Northern Ireland Council challenged the stereotype that deaths are only among dependent drinkers:
People think about alcoholics and conjure up an image of somebody who’s down on their luck or maybe on the street. That’s not every alcoholic; that’s not every dependent or problem drinker. There are many professionals, people going out to work every day who are drinking heavily in the evening and are managing to maintain their day-to-day life. But that doesn’t mean that their drinking is any less problematic.
Calls for minimum unit pricing (MUP)
These shocking statistics have prompted urgent calls for MUP to be introduced in the country.
“Urgent action” is needed to prevent these deaths, the Alcohol Health Alliance said in a letter to the First and Deputy Ministers.
Professor Sir Ian Gilmore, AHA Chair, said:
The evidence is clear that MUP reduces consumption and saves lives, particularly in the communities that suffer the greatest levels of alcohol harm. With deaths rising and inequalities widening, the need for decisive action has never been more urgent.
Dr Joy Watson, chair of the Addictions Faculty, Royal College of Psychiatrists NI, said:
It’s Northern Ireland’s shame that alcohol deaths are at an all-time high… The government need to listen to medical experts as MUP could save lives and cut NHS costs. There is no hidden agenda – only public health gain.
Mike Nesbitt, the fifth health minister to try to introduce MUP, has said time is “quite rapidly” running out for the Executive to introduce the policy. Ironically, despite the DUP’s Edwin Poots first proposing the policy in 2012, it is the DUP that is preventing the policy from progressing.
A spokesperson for the DUP said the party will engage with the health minister to “achieve proposals which can both achieve consensus and make the meaningful impact on alcohol related harm that everyone wants to see”. They have claimed that the measure is unfair on people from deprived backgrounds.
Dr Sheila Gilheany of Alcohol Action Ireland joined Sunday Politics Northern Ireland and said that the DUP has seen all of the evidence, but are claiming they don’t understand it. She said:
If they have questions, we’d be more than happy to answer them. We wouldn’t be pushing for something if we didn’t see that it would make a difference.
She added “wouldn’t the DUP like to point to how many lives they’ve saved next year?”
Welsh Senedd votes to continue and increase MUP

Members of the Senedd (Welsh Parliament) have voted to continue MUP and to bring the price in line with Scotland’s rate of 65p.
Research by the Sheffield Addictions Research Group found that increasing the price could prevent more than 900 deaths over the next 20 years and prevent the number of higher risk drinkers by nearly 5,000.
Sarah Murphy, Minister for Mental Health and Wellbeing, said:
Cheap, high-strength alcohol disproportionately affects hazardous and harmful drinkers. The evidence is clear – minimum unit pricing works. We have today taken a decision which will save lives and help protect many people from the harms caused by drinking too much alcohol.
Andrew Misell, Director for Wales at Alcohol Change UK, welcomed the policy, commenting:
Inflation has steadily eroded the impact of the minimum unit price since it was introduced in 2020. This increase restores the policy’s effectiveness and ensures it can continue to reduce the availability of the cheapest, strongest alcohol that causes the most harm.
Clive Birkby, Wales president of the Federation of Independent Retailers, told the BMJ it had no objection to the MUP changes:
In the past, supermarkets have sold alcohol as super-cheap loss leading products, something which is damaging to small shops and also to those advocating responsible consumption.
We have highlighted concerns, though, for how this policy will impact our members who are close to the border with England, given that England does not have MUP.
We will continue to monitor the impact of this policy change and what it might do to reduce problem drinking and the health and social impact of that—though we will repeat our call for the Welsh and Westminster governments to provide more information about responsible drinking through better education.
The price change regulations will come into effect from 1 October 2026.
DHSC says it is “categorically untrue” that industry lobbying watered down 10 Year Health Plan
The Department of Health and Social Care (DHSC) has called claims in a BMJ news piece about IAS’s Now you see it, now you don’t report “unfounded” and “categorically untrue”. The report found that the alcohol industry had aggressively lobbied the UK Government before alcohol marketing restrictions were removed from the 10 Year Health Plan. DHSC said:
It is categorically untrue that any policy content of our 10 year health plan was changed by lobbying. We engage with industry partners and these are unfounded allegations based on a leaked, unfinished version of our health plan.
The government recognises the harms associated with excessive drinking and has taken crucial steps in the health plan to support people to make healthier choices.
Despite this, DHSC failed to explain why the department went from stating that partial alcohol marketing restrictions were in the draft of the Plan to removing any mention of such restrictions.
Jeff Collin, professor of global health policy at the University of Edinburgh, told the BMJ that:
It’s clear that the alcohol industry got what it wanted out of this process. The consequences are likely to be pretty dreadful…
In an opinion piece for LabourList, Labour MP for Lancaster and Wyre Cat Smith wrote:
At a time of shocking levels of alcohol harm, it is deeply troubling that the alcohol industry was able to exert this kind of influence on a flagship NHS policy. It also departs from the needs of the public. Unfortunately, our communities will pay the price.
In response to a written parliamentary question, Public Health Minister Ashley Dalton said that DHSC will continue to work with DCMS to “consider if additional statutory restrictions on marketing and advertising are needed to reduce alcohol related harms”.
However, in the same answer the minister said that there is a balance to be struck between reducing alcohol harms and supporting economic growth.
Reform UK publishes 5-point plan to “save Britain’s pubs”
Reform UK, which is the leading political party in most polls, has published a plan to stop the closure of Britain’s pubs, claiming that “the Conservatives, and now Labour, have facilitated the closure of thousands of pubs over the last decade”.
The plan would:

The biggest public health risk would be the cut to beer duty – particularly if extended to all alcohol products across both the on- and off-trade. Such a move would do little to support pubs and would likely harm them, as across-the-board duty cuts disproportionately benefit supermarkets, where duty makes up a larger share of the final price.
Reform says it would fund these cuts by reinstating the two-child benefit cap, which they claim would raise £3 billion by 2029-30.
Tim Martin, owner of JD Wetherspoon, said Nigel Farage has a:
massive advantage in that he’s a genuine piss artist. He genuinely likes a sherbet, which, when it comes to pubs, people can tell that.
Reform is streets ahead in its pubs policy.
However, others were very critical, with many on social media arguing that increasing child poverty wouldn’t be worth a pint getting slightly cheaper. In a Commons debate, Labour’s John Slinger said that the plan was “populist policy hokey-cokey” and Labour’s Dr Jeevun Sandher said parents would not appreciate getting 5p off each pint knowing it would make more children hungry.
In The Mirror, progressive think tank IPPR said that the numbers didn’t add up, as the loss of VAT would be around £5.6 billion. Professor Ashwin Kumar, director of research and policy at IPPR, and a former advisor to Gordon Brown, said:
Hospitality needs help, but this shouldn’t be paid for off the backs of some of the poorest in society who need this support so their children can thrive. This is also not a fiscally neutral plan as is claimed. The costs of halving VAT alone would be much more than the claimed £3billion saving from reinstating the two-child limit. In reality, this is an unfunded tax cut which someone will have to pay for.
Shadow Chancellor Mel Stride said that it’s:
More fantasy numbers from Reform” that would “blow a £10billion hole in the public finances” and were “totally irresponsible… Their sums just don’t add up. How can anyone trust a word Reform say if they won’t explain where any of it comes from?
In response, a Reform spokesperson said:
Under Conservatives, pubs were driven to the brink of extinction through punitive taxation and sky high energy costs. Their current plans clearly don’t go nearly far enough to save British pubs while Reform UK’s have been welcomed by two of Britain’s biggest pub operators. Minor party Mel would be better off apologising for the 10,400 pubs which closed under the Tories.
Stronger alcohol warnings could boost public awareness – and support for more effective policies
Two new studies highlight why the UK’s plans to strengthen alcohol labelling matter. A nationally representative US study in Addictive Behaviors found that while 52% of US drinkers noticed the current health warning, only 27% had read it in the past month – and just 4% could recall all five warning topics. Most remembered pregnancy risks, far fewer recalled broader health harms, prompting calls for stronger, rotating warnings.
Meanwhile, a 2024 survey in the European Journal of Public Health across five EU countries found that awareness of alcohol’s link to cancer was associated with greater support for tougher policies, including pricing and availability measures. Clearer, more prominent health warnings could therefore both inform consumers and build support for effective alcohol control.
Cancer Plan published, but no new commitments on alcohol
The UK Government published its National Cancer Plan for England in early February, which commits to ensuring three in four people diagnosed with cancer from 2035 are cancer-free or living well after five years.
The plan mainly focuses on how diagnosis and treatment can be improved, by expanding robot-assisted surgery, genomic testing, and treatment centres.
It also states that the government is taking action on the causes of cancer, namely a generational ban on smoking and a ban on junk food ads before 9pm.
There are no new commitments on alcohol, although it is acknowledged as a cause of cancer in the plan, and improved labelling is mentioned.
Sarah Woolnough, Chief Executive of the King’s Fund, reflected on the plan, stating that it:
does a sound job on analogue to digital and hospital to community, it does less well on the sickness to prevention shift, a recurrent theme in government policy.
And Lib Dem Baroness Walmsley said in the Lords that the Plan was a missed opportunity to introduce minimum unit pricing to help tackle alcohol-related cancers.
Professors Bernard Rachet, Ajay Aggarwal, and Martin McKee were much more damning in the BMJ, writing that it “reads more convincingly as an industrial strategy” than a health reform programme.
While it promises earlier diagnosis, personalised care, and faster access to innovation, they say improvements to health outcomes appear “almost secondary in its purpose”.
Without sustained investment in staff, infrastructure and health system reform, they conclude, the plan risks serving “economic objectives more effectively than population health”.
Alcohol Toolkit Study: update
The Alcohol Toolkit Study is a long-running survey of alcohol consumption in England, Scotland, and Wales. The English monthly data have been collected since March 2014, and the Scottish and Welsh data from mid-2021. Each month involves a new representative sample of adults aged 16 and over.
You can find further charts and data for each country here:
· England
· Scotland
· Wales
The following charts are a snapshot of the prevalence of risky drinking by social grade.
Prevalence of increasing and higher risk drinking (AUDIT-C)
Risky drinking defined as those scoring AUDIT-C ≥5
ABC1: Professional to clerical occupation; C2DE: Manual occupation
England
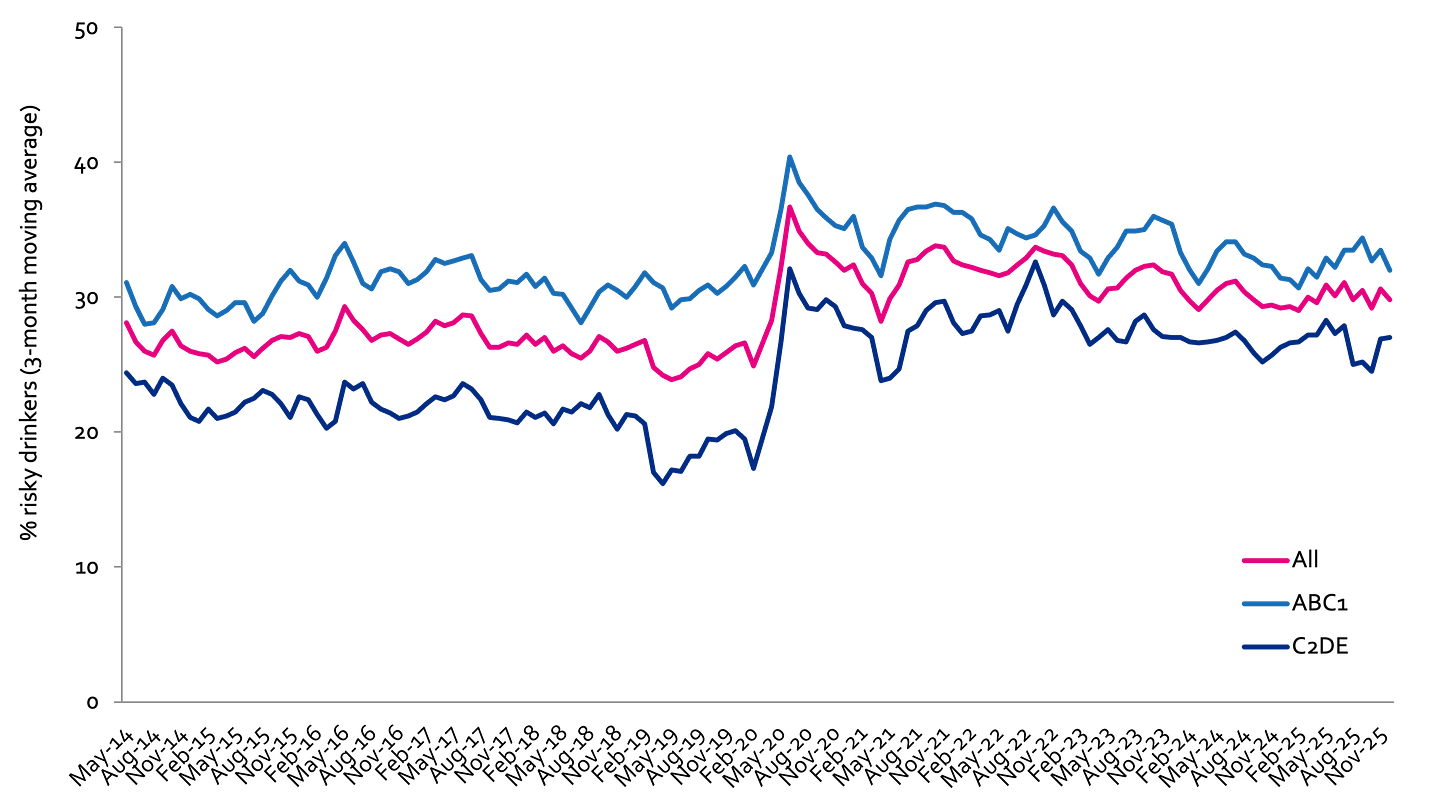
Scotland
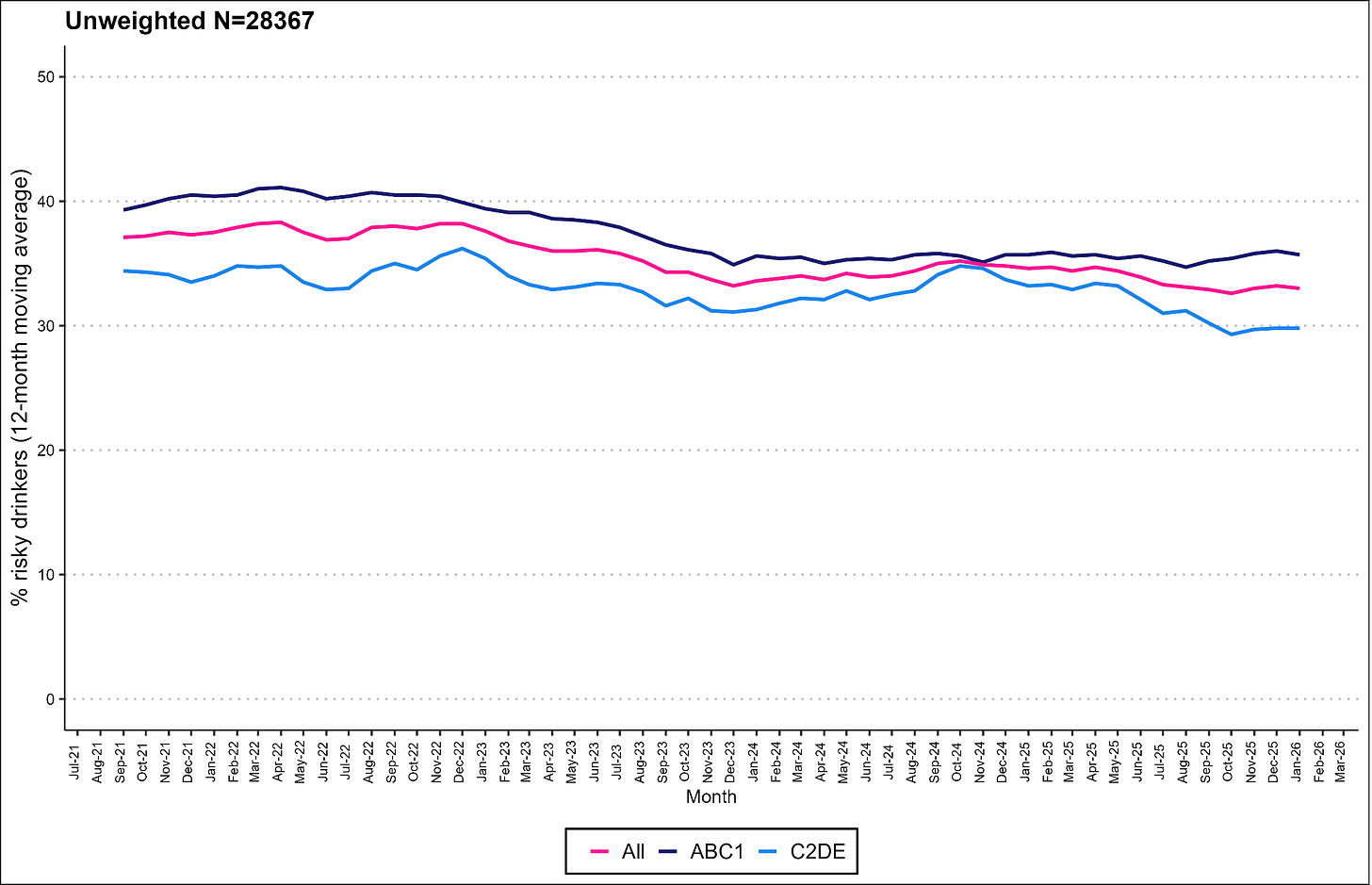
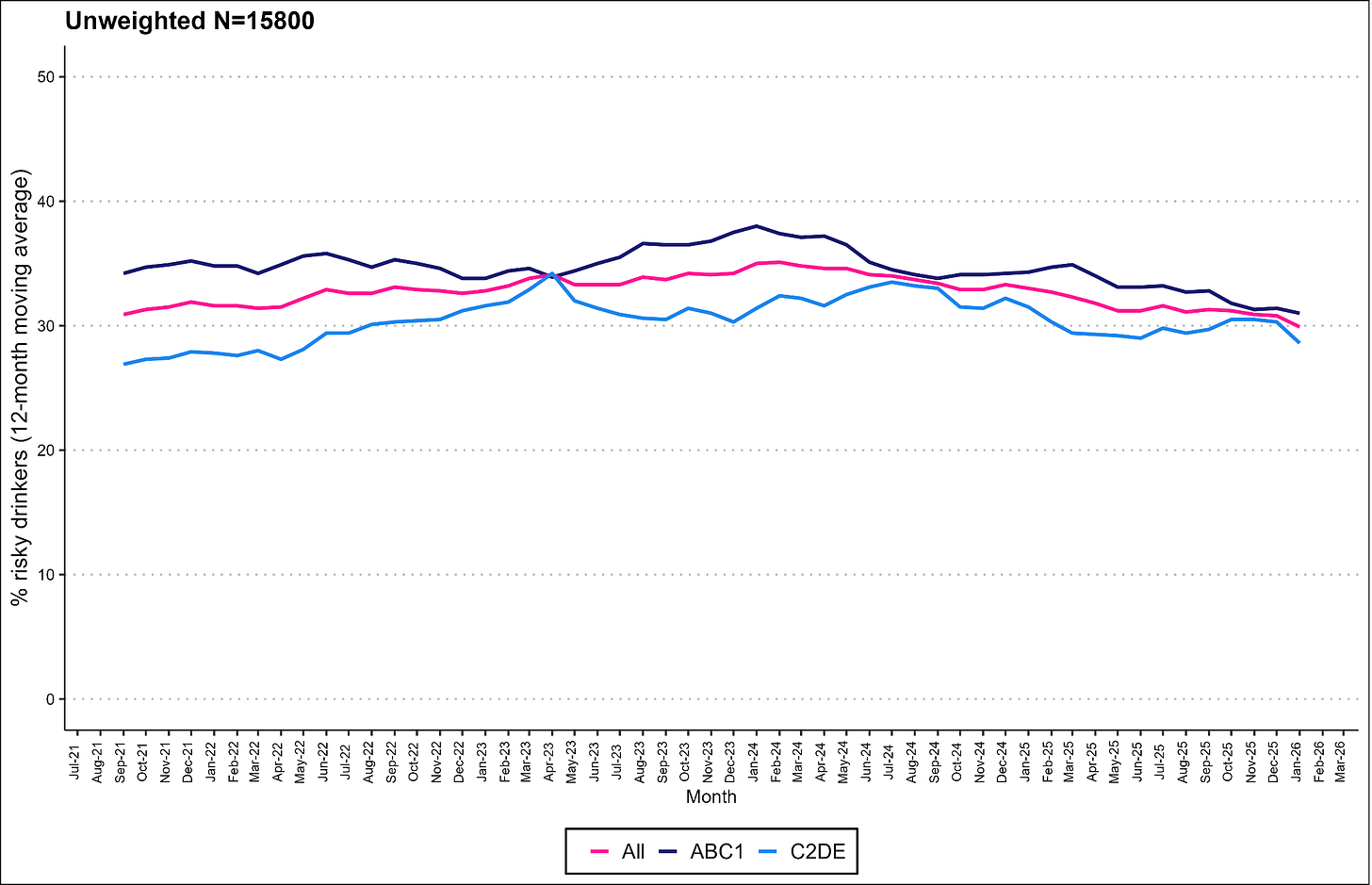
Wales
Podcast
Our monthly podcast features interviews with experts from across the sector.
Humanising Healthcare’s Conversation Café: transforming medical education
Dr Hugo Jobst –
Humanising Healthcare
Dr Seonaid Anderson –
Consultant Psychiatrist
Allan Houston –
Glasgow City Council

