In this month’s alert
Big Alcohol: Explained – IAS launches new film series

IAS is excited to launch a new film series called Explained, which will include nine explanatory films featuring topic experts.
Our first to be published is Big Alcohol: Explained, featuring Professor Mark Petticrew (LSHTM), Dr Gemma Mitchell (University of Stirling), and Dr Aveek Bhattacharya (Social Market Foundation).
The film explains who the main players are in the multinational alcohol industry, what their growth and profit strategies are, how they influence health policy and shift blame of harm onto consumers, and why they damage the economy.
The films will be 15-20 minutes in length, in order to provide a succinct but relatively thorough explanation of each of the topics. The next two in the series will be ‘The Price of Alcohol: Explained’ and ‘The Marketing of Alcohol: Explained’ and will be published in the coming months.
We hope the films will be useful for those wanting to learn about alcohol research and policy. We would love your support in signposting to these films and sharing with colleagues you think would find them useful. They will be hosted on each related page on our Alcohol Knowledge Centre, as well as on our YouTube channel.
Alcohol deaths in Scotland reach highest level in 14 years
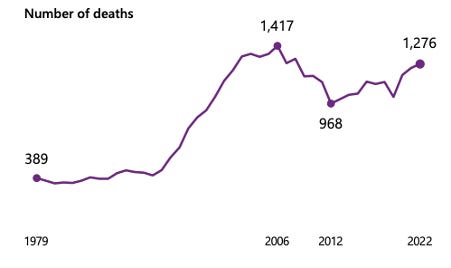
The latest figures from the National Records of Scotland (NRS) show 1,276 people died from alcohol-specific causes in 2022. This is 2% higher than 2021 and the highest number since 2008.
Although the gap in mortality rates between the most and least deprived areas has narrowed, rates are still 4.3 times as high in the most deprived areas.
The average rate of mortality was 22.9 deaths per 100,000 people in 2022, up from 22.3 the previous year. NRS said it did not consider the rise to be ‘statistically significant’.
Professor Sir Ian Gilmore, chair of the Alcohol Health Alliance, said:
“The crushing news that the number of people who lost their lives to alcohol in Scotland has risen again is a grave reminder that we are in the midst of a public health crisis with alcohol.
“Each of one of the 1,276 deaths was entirely preventable and presents a tragic loss for the loved ones and communities left behind.”
Justina Murray from Scottish Families Affected by Alcohol and Drugs said: “We are definitely not doing enough.”
She called for more action such as better access to recovery services and an increase in the minimum price of alcohol from 50p to 65p.
The Minister for Drugs and Alcohol Policy, Elena Whitham, also commented on minimum unit pricing (MUP):
“If we didn’t have minimum unit pricing in place, I think that the deaths that we would be seeing today would have been higher. We know that the evaluation from Public Health Scotland shows that there has been an estimated hundreds of people whose lives have been saved by minimum unit pricing.”
Rise among women only
Dr Alastair MacGilchrist, chairman of Scottish Health Action on Alcohol Problems, highlighted how the rise was in deaths among women, with mortality among men remaining the same. In a recent blog, he discussed why this might be:
“The gender-specific mortality figures reveal that the reduction in deaths in 2019 – which followed the introduction of MUP – applied only to men; there was no reduction in female deaths. Sheffield Alcohol Research Group have modelled the possible effects of MUP at different levels on men and women. Their results, published in 2021, predicted that MUP at 50p would not reduce female deaths – whereas a higher level (the price modelled was 70p) would do so.”
Dr MacGilchrist also said that it is essential that the Scottish Government addresses this public health emergency:
“It is vital that policies such as MUP remain in place to continue to reduce alcohol-related harms. The level at which MUP is set should be raised to at least 65p to maintain its benefit.
“Alongside this, the Scottish Government must address the wider availability and marketing of alcohol, in order to tackle the inescapable exposure to alcohol experienced by children and other vulnerable groups, such as people in recovery.”
Scottish Labour public health spokesperson Carol Mochan said:
“This is a public health emergency on the same scale as Scotland’s drug death crisis, and both are the legacy of the SNP’s shameful cuts to Drug and Alcohol Partnerships.”
Labour MSP Katy Clark agreed, and stated that:
“While minimum pricing has undoubtedly played a role in reducing alcohol-related health inequalities, it is not the silver bullet to addressing this issue. We need to see investment in alcohol recovery services and more action taken to tackle the marketing, availability, and price of alcohol across Scotland.”
Marketing restrictions not scrapped
On the topic of marketing, Elena Whitham stated at the end of August that marketing restrictions are not off the table in Scotland and that there were still 3,000 responses to analyse:
“Whilst we are back to the drawing board – that doesn’t mean that it’s cancelled and it’s not going anywhere. It just means that we’re going to have a slightly different focus on it, but my focus on it is absolutely from a public health perspective.”
Laura Mahon, deputy chief executive of Alcohol Focus Scotland, said it was frustrating that Scotland does not have full powers over alcohol marketing anyway.
“We’ve got two governments that are in completely different places when it comes to strategies to reduce alcohol harm.
“The Scottish Government has made tackling alcohol harm one of its priorities and at Westminster things are really far behind where we are in Scotland. It is frustrating that we don’t have more of that power here I think, but the priority right now is persuading the Scottish Government to use the powers it has.”
Scottish Government proposes raising minimum unit price to 65p in new consultation
The Scottish Government has published a new consultation regarding the future of MUP. The consultation asks whether MUP should continue as a measure to reduce alcohol harm, and if so, at what level. The document states that:
“…the Scottish Government is satisfied that there is a strong case to continue with MUP…The Scottish Government also proposes the level of minimum unit price is revised to 65ppu to provide a proportionate response to tackling alcohol harms. It strikes a reasonable balance between public health benefits against the effects of any intervention in the alcoholic drinks market and subsequent impact on consumers.”
Elena Whitham said:
“We believe the proposals set out in this consultation strike a reasonable balance between public health benefits and any effects on the alcoholic drinks market and subsequent impact on consumers, but we want to hear from all sides and urge everyone to take the time to respond.”
The BBC looked at how prices would change with a rate of 65p:
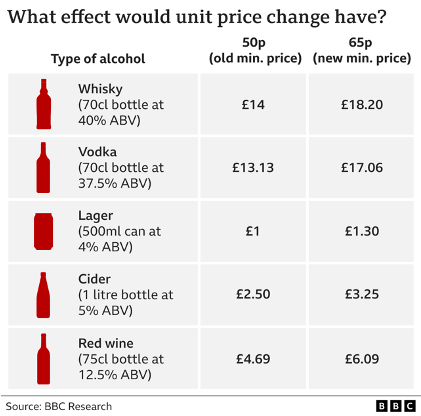
IAS would encourage people to respond to the consultation using the online form here. There are only three questions so it shouldn’t take more than 5 minutes.
The Scottish Government’s report on MUP published alongside the consultation recognises that the measure has reduced alcohol-related deaths and hospitalisations in the country, particularly in the most deprived areas.
IAS chief executive, Dr Katherine Severi, welcomed the news and called on the UK government to follow Scotland’s lead:
“We know that drinking patterns changed during the pandemic, with those drinking at harmful levels consuming more. With deaths from alcohol at an all-time high, effective policies to reduce harm are therefore needed more than ever.
“The more evidence that comes out from Scotland showing how minimum unit pricing saves lives and improves health equity, the more it highlights the UK government’s failure to act. Over the past decade, health inequalities have spiralled. To have a simple and evidence-based policy that directly reduces this inequality is a gift; a gift that continues to be disregarded. The UK government must follow Scotland’s lead to avoid England becoming the sick nation of the UK.”
The chair of the Alcohol Health Alliance, Professor Sir Ian Gilmore, also demanded action from the Westminster government:
“…there is a message for the politicians in Westminster too; over 250 lives every year are being saved in Scotland because of MUP, while the number of avoidable deaths in England continue to rise. The UK government can no longer, in good conscience, sit on the evidence. It must act on its promise to review MUP in England now.”
Dr Alastair MacGilchrist said this was a significant moment in the journey to reduce alcohol harms in Scotland, and that all MSPs must get behind it:
“While MUP must be part of a range of policies to reduce alcohol harms in Scotland, including restricting alcohol marketing and prioritising access to treatment, we must ensure that its ability to save lives is not eroded by inflation.”
New report highlights erosion of MUP by inflation
A new report from the University of Sheffield – published to coincide with the consultation release – has found that the minimum unit price, which was set at 50p per unit when it was introduced by the Scottish government in May 2018, is now equivalent to 41p per unit after adjusting for the effects of subsequent inflation.
The report had two main conclusions:
“First, the erosion of the real-terms value of the MUP by high levels of inflation is likely to increase alcohol related harm. Adjusting the level of the MUP to account for inflation is therefore important to maintain its public health impacts.
“Second, the long-term effects of the COVID-19 pandemic are also likely to lead to increases in alcohol-related harm that will cancel out some of the beneficial impacts of MUP.”
Westminster’s response
In a written Parliamentary Question, Labour MP Dan Carden asked whether the Home Office plans to consult on introducing MUP in England. Minister Chris Philp responded that:
“The Government maintains an interest in the impact of minimum unit pricing in Scotland and will consider the findings from the outcome report in due course.”
184,000 preventable cancers diagnosed in 2023 will cost £78 billion – Podcast feature
The consultancy Frontier Economics published a report in mid-September that found there will be 184,00 preventable cancers diagnosed this year, at a cost of £78 billion to the UK economy.
The causes of preventable cancers included alcohol consumption, smoking, poor diet, and exposure to UV radiation.
The total cost, which is equivalent to 3.5% of the UK’s Gross Domestic Product (GDP), includes £40 billion in lost productivity, £30 billion in costs to the individual, £3.7 billion NHS costs, £3.4 billion cost to families and carers, and £1.3 billion in social care costs.
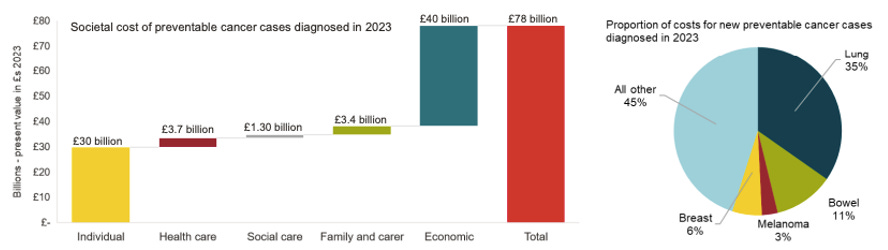
One of the report authors, economist Nicholas Woolley, joined our podcast and called for more to be done to reduce alcohol consumption across the population. He also highlighted that the £78 billion figure was likely a slight underestimate.
In The Guardian on 10 September, the BMA called for the government:
“To reduce the availability and attractiveness of products such as alcohol, tobacco and junk food that contribute to a large number of preventable diseases, including some cancers.”
IAS head of research, Dr Sadie Boniface, explained that:
“Since 1988, alcohol has been classified as a class 1 carcinogen by the International Agency for Research on Cancer (part of the World Health Organization) alongside tobacco and asbestos. In 2020 alone, almost 17,000 cancers due to alcohol were diagnosed in the UK.”
Cancer Research UK’s chief executive Michelle Mitchell, called for bold action to reduce smoking rates, and said that:
“This report is a stark reminder of the countless lives that could be saved by preventing cancer and a call to the UK government that health prevention strategies are key to relieving pressures on our NHS and economy.”
A DHSC spokesperson said:
“We have introduced calorie labelling, announced a £40m pilot to give eligible patients living with obesity access to effective obesity drugs, and will help a million smokers across England quit by giving them a free vaping starter kit. There are record numbers of cancer checks happening in the NHS and our major conditions strategy will set out further plans to tackle the main causes of ill-health.”
Dire need for labels on alcohol
The Guardian followed up its publicising of the report later that week, by calling for public awareness campaigns and improved labelling to tackling alcohol harm and obesity.

The World Cancer Research Fund (WCRF) said that mass media campaigns are needed to tackle the widespread lack of awareness that alcohol and being overweight are both major causes of cancer.
Dr Panagiota Mitrou, the WCRF’s director of research, said:
“History shows that sometimes very graphic, hard-hitting tactics in campaigns – even images that risk upsetting some people – are necessary to alert the public to the dangers of unhealthy behaviour.”
Dr Boniface said that warning labels on alcohol products would improve the very low levels of awareness that alcohol caused cancer:
“The fox has been left in charge of the hen house, with the alcohol industry self-regulating its own product labelling. A couple of years ago the government promised a consultation on alcohol labelling but it is yet to materialise.”
As recently as 13 September, the UK government was still repeating that it had committed to consulting on alcohol calorie labelling. The consultation would provide an opportunity to highlight other aspects of labelling that should be required, such as prominent health warnings.
In related news
A study published at the beginning of September by the University of Edinburgh and the Zhejiang University School of Medicine in China found that alcohol, smoking and obesity have led to a surge in cancer cases among younger age groups.
Between 1999 and 2019, cancer cases increased by 79% in people aged under 50.
The study looked at 29 different cancers across 204 counties and regions examining new diagnoses, deaths, health consequences and risk factors in people aged 14 to 49. The regions with the highest rates of early-onset cancers were North America, Australasia and Western Europe.
Adfam report shows Drug Strategy funding not filtering through to families – Podcast feature

Adfam – a charity that supports family members and friends of those affected by alcohol and other drug problems – published findings of its new report: ‘State of The Family Support Sector 2023’. The report surveyed over 100 service providers, to understand current trends, developments, strengths and challenges facing those working to support family members.
The findings highlight the negative impact of the pandemic, as well as issues around funding. It found:

Vivienne Evans, Adfam’s chief executive, explained that:
“Very little of the money the government has pledged appears to be making its way through to the family sector.”
Listen to our podcast to hear from Adfam’s Policy and Communications Lead Robert Stebbings, who discussed the challenges facing family-specific support services.
Scottish Government supports the Scotch Whisky Association’s drinking campaign
The Scottish Government has said it will support the Scotch Whisky Association’s (SWA) ‘Made to be Measured’ campaign. The campaign purportedly aims to raise awareness of the alcohol content of drinks and the chief medical officers’ low risk drinking guidelines.
First Minister Humza Yousaf said:
“The whisky industry’s willingness to raise awareness of alcohol misuse and the health risks associated with high consumption of alcohol, through the SWA’s ‘Made to Be Measured’ campaign, is very welcome.
“This is just one of the key areas of partnership that the Scottish Government and whisky industry can work together on – and I look forward to furthering our productive partnership on shared priorities such as the transition to net-zero, global trade and investment, and economic growth.”
Some have been quick to point out that the ‘responsible drinking’ campaign includes cocktail recipes on its landing page. Some of the imagery doesn’t include the low risk guidelines and clearly resemble adverts, such as the following:

The Scottish Government’s support of the campaign also seems to contravene it’s 2018 Alcohol Framework, which states that it will not work with the alcohol industry…
“…on health policy development, on health messaging campaigns or on provision of education in schools and beyond the school setting”.
England’s suicide prevention strategy includes ‘reducing population level alcohol consumption’
The Department of Health and Social Care published its Suicide Prevention 5-year cross-sector strategy on 11 September. Among other priorities, the strategy identified addressing the following social determinants of health: physical illness, financial difficulty and economic adversity, harmful gambling, substance misuse, domestic abuse, and social isolation and loneliness.
Focusing on alcohol, the strategy acknowledged the importance of “reducing excessive alcohol consumption at a population level and instances of acute intoxication”. It went on to state that the reform of alcohol duty is a way to “target problem drinking” by taxing products by strength.
“HM Treasury and HM Revenue and Customs, with support from DHSC, will evaluate the impact of alcohol duty reforms, including on population-level rates of alcohol consumption and levels of alcohol harm.”
Alcohol Toolkit Study: update
The monthly data collected is from English households and began in March 2014. Each month involves a new representative sample of approximately 1,700 adults aged 16 and over.
See more data on the project website here.
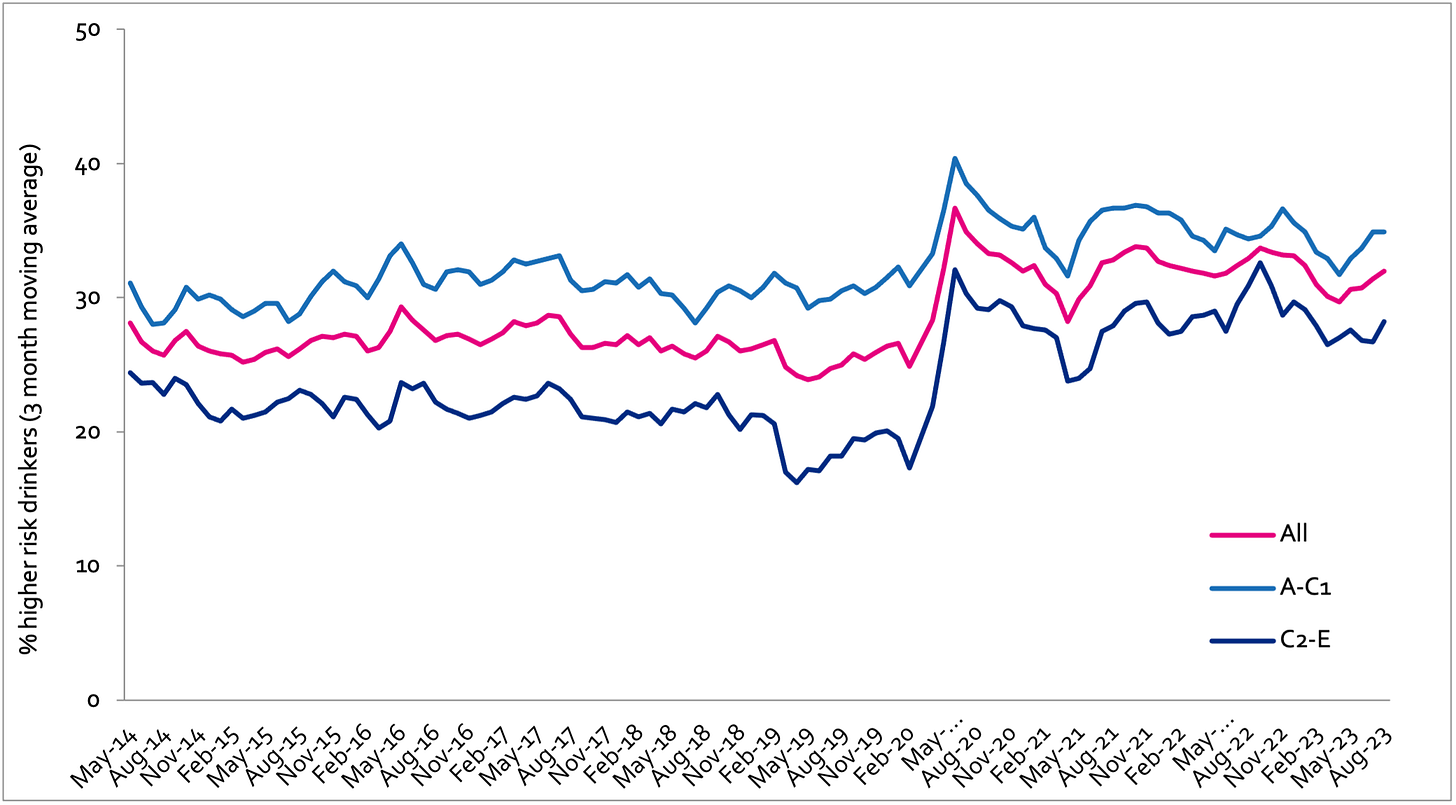
Prevalence of increasing and higher risk drinking (AUDIT-C)
Increasing and higher risk drinking defined as those scoring >4 AUDIT-C. A-C1: Professional to clerical occupation C2-E: Manual occupation
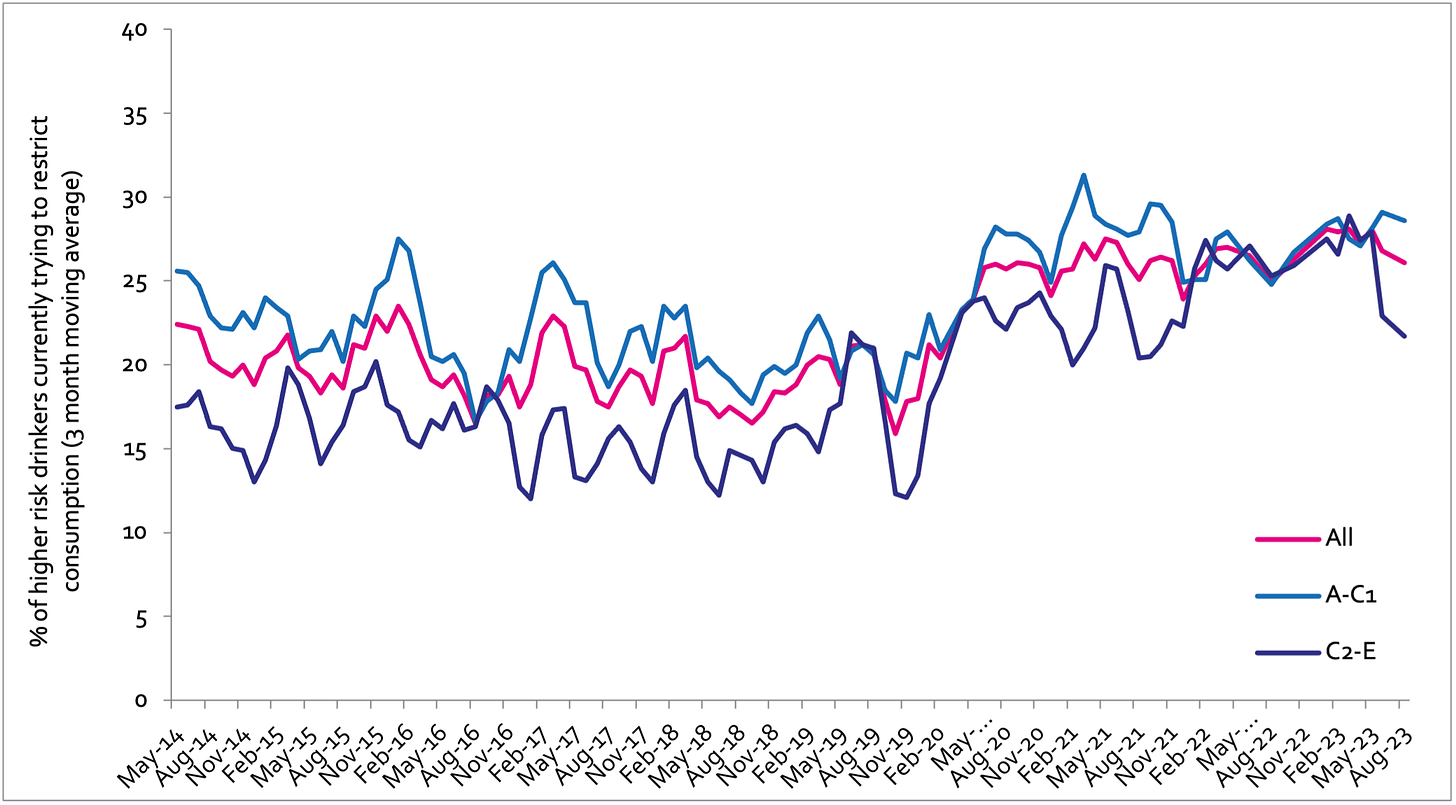
Currently trying to restrict consumption
A-C1: Professional to clerical occupation C2-E: Manual occupation; Question: Are you currently trying to restrict your alcohol consumption e.g. by drinking less, choosing lower strength alcohol or using smaller glasses? Are you currently trying to restrict your alcohol consumption e.g. by drinking less, choosing lower strength alcohol or using smaller glasses?
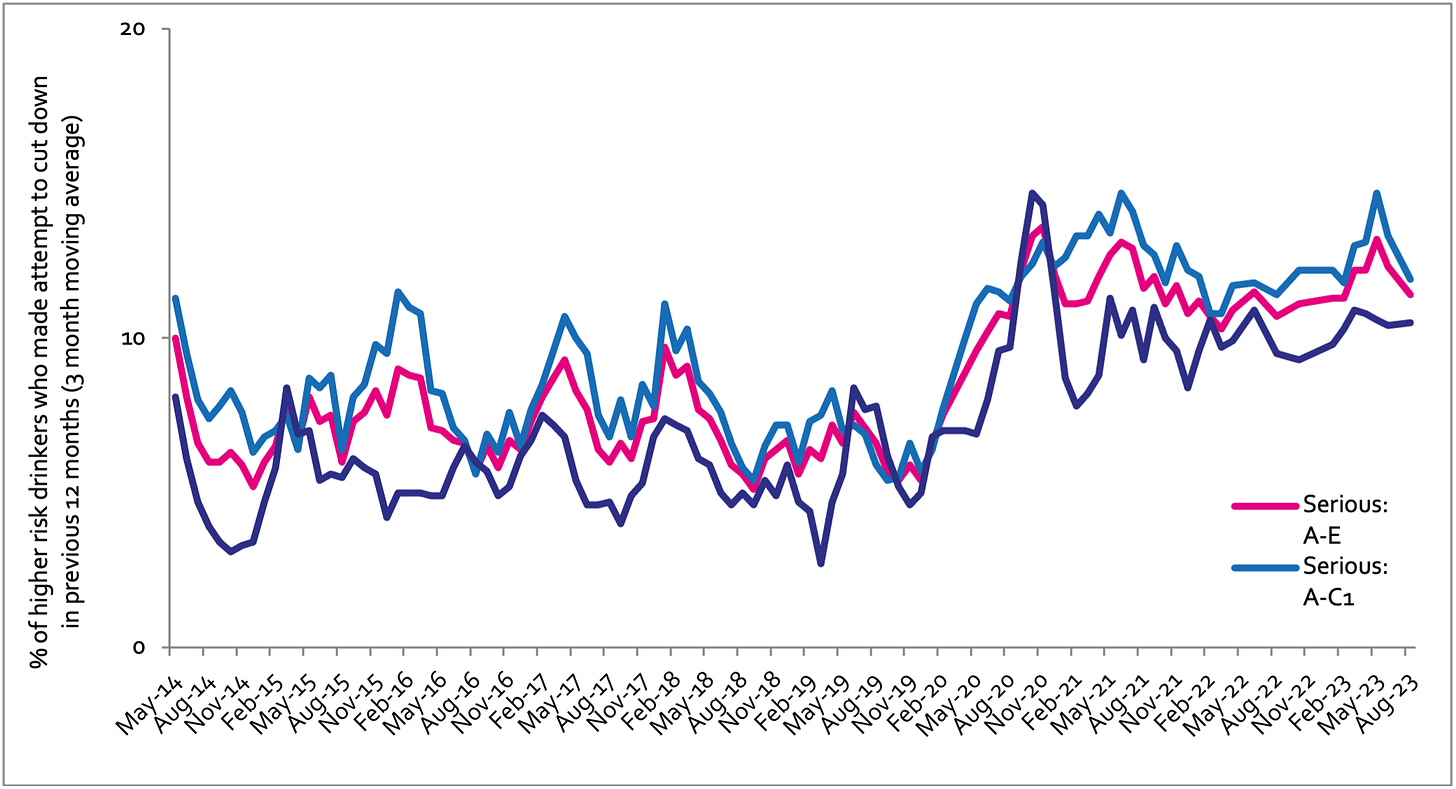
Serious past-year attempts to cut down or stop
Question 1: How many attempts to restrict your alcohol consumption have you made in the last 12 months (e.g. by drinking less, choosing lower strength alcohol or using smaller glasses)? Please include all attempts you have made in the last 12 months, whether or not they were successful, AND any attempt that you are currently making. Q2: During your most recent attempt to restrict your alcohol consumption, was it a serious attempt to cut down on your drinking permanently? A-C1: Professional to clerical occupation C2-E: Manual occupation
Podcast
Our monthly podcast features interviews with experts from across the sector.
Getting to SAFER, Faster: Reflections on GAPC 2026
Laura Cury –
ACT Health Promotion, Brazil
Emma Thompson –
University of Edinburgh & IAS

